When it comes to surgical procedures, your pet’s comfort and safety is our utmost concern, and we don’t cut corners.
High Standards of Care
We strive to provide the level of care, service, and medically-trained, licensed staff we would want for our own pets or children. There are standards of care we will not breach to make a procedure less expensive. If needed, we may provide payment plans for established clients to spread out the cost of a procedure.

Individualized Care for Your Pet
To provide your pet with individualized care, our surgeries and dental procedures are scheduled, planned, and performed individually, not as an assembly line.
Customized Anesthetic Plan
Before we begin a procedure, we provide a courtesy pre-anesthetic doctor exam (a $63 value) where the doctor assesses your pet’s current health status and writes an individualized anesthetic and pain management plan.
For maximum safety and comfort, we customize the plan for each pet, taking into account the pet’s age and health status, as well as the type, duration and severity of pain that may accompany a procedure.
Pain Management Plan
We provide a multi-modal pain management to deliver consistent, reliable comfort using different classes of drugs that work together to provide pain management at lower, safer doses.
A typical multi-modal pain management plan may include:
- pain injections before, during, and after the procedure for extra comfort
- gas anesthesia and oxygen (via endotracheal tube for airway protection)
- acupuncture to improve anesthesia
- local anesthesia at the site of the incision or dental extractions
- a dermal patch providing round-the-clock pain medication for three days after the procedure
- oral pain medications to be given at home during the healing period
Pre-Anesthetic Laboratory Screening
For the safety of your pet and to assist in planning the procedure, we require pre-anesthetic laboratory screening within 30 days of a procedure to assess your pet’s internal organ functions.

We have negotiated with our reference lab to offer a mini panel (sufficient for most, but not all pets) at the lowest possible price. Lab screening also serves as wellness screening for your pet, setting an individualized baseline to which we can compare any future lab results.
General Anesthetic Best Practices
During all general anesthetic procedures, we place an IV catheter and provide intravenous fluids at a rate individually calculated for each pet, providing support to your pet’s cardiovascular system and kidneys. The catheter also provides immediate intravenous access in case of emergency.
Dedicated Surgical Veterinary Nurse
A separate trained and experienced veterinary nurse is dedicated to your pet to monitor anesthesia and vital signs throughout the entire procedure and recovery period. The technician carefully and continuously assesses blood pressure, oxygen saturation, pulse rate, respiration, tissue perfusion, comfort level, and body temperature.
Monitoring is accomplished through subjective methods (e.g., clinical appearance) and objective methods (e.g., electronic systems).
In anesthesia, seconds count. Immediately recognizing and responding to a change in patient parameters provides better patient outcomes, reduces stress during the procedure, and may help minimize overall procedure time.
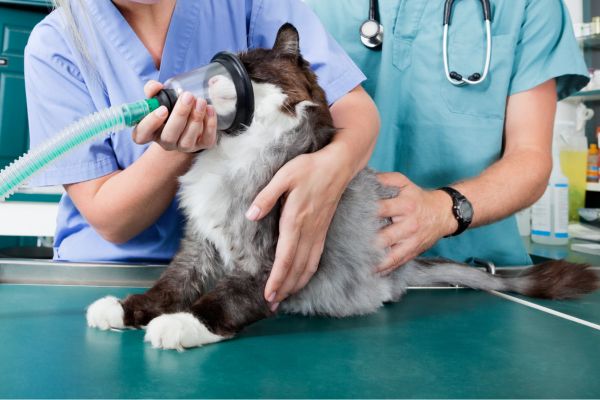
Some clinics expect the person performing the procedure to also monitor anesthesia, but having a separate person solely responsible for anesthesia increases safety.
Sterile Surgical Suite
Our doctors perform surgery in a separate, sterile surgical suite and are capped, masked, gloved, and gowned. The anesthetic nurse is also capped and masked. Some clinics do not insist upon this level of sterility.
Courtesy Grooming Services
We provide courtesy grooming services while your pet is under anesthesia, including a nail trim and anal gland express (a $50 value) – two procedures many pets aren’t too enthused about while awake.
Padded E-Collar
We budget for and encourage the use of an Elizabethan collar (e-collar) for many surgeries to help keep your pet from licking his/her incision, causing self-trauma, infection, and pain. We have new padded collars that are more comfortable and better accepted by pets.
Discharge Appointment
We write individualized home care instructions, taking the time at your discharge appointment to review them with you and answer any questions you may have before your pet goes home.
Courtesy Re-Evaluation Exam and Suture Removal
We provide a courtesy re-evaluation exam (a $45 value) with the doctor within 7 days to check your pet’s healing progress. We also provide a courtesy suture removal appointment, if necessary, 10-14 days after a procedure.
All-Encompassing Cost Estimates
No one likes unwelcome surprises or tense conversations, so we try to provide an all-encompassing, “soup to nuts” treatment plan and cost estimate. We attempt to anticipate all costs associated with a procedure, while maintaining our standard of care (and providing courtesy services we think you’ll appreciate).
Cost Estimates for Non-Elective Procedures
With non-elective procedures, we may provide a cost range to attempt to encompass unknowns, and we’ll call you during the procedure if additional unknowns arise.
When asked for a cost quote, we don’t just quote for the procedure, as some clinics do, then surprise you with the cost of take-home medications, supplies, and recheck appointments that add to the total. We provide that information right up front. And we don’t cut corners.